How Common Is Periodontitis in Dogs, and Who Is Most at Risk?
Canine periodontitis risk factors include a combination of breed, age, body size, head shape and home care habits. Here is a quick summary of the most significant ones:
| Risk Factor | Key Detail |
|---|---|
| Small body size | Small breeds are 2 to 3 times more likely to develop periodontal disease than large breeds |
| Age | Most dogs over 5 years have significant periodontitis |
| Brachycephalic head shape | Ranked as the highest-weighted single risk factor by veterinary practitioners |
| Overweight body condition | Overweight dogs have greater odds of diagnosis across all breeds and sizes |
| Poor oral hygiene | Plaque recolonises tooth surfaces within 24 hours of cleaning |
| Breed genetics | Yorkshire Terriers, Poodles and Greyhounds show notably high prevalence |
Periodontal disease is the most common health problem in dogs. Studies suggest that between 80 and 90 percent of dogs over the age of three already have some degree of it. Yet most owners never realise there is a problem, because dogs instinctively mask pain and the early stages are invisible without a professional examination under anaesthesia.
The disease starts with plaque, a thin bacterial film that forms on teeth within hours of cleaning. Left unmanaged, it hardens into tartar, triggers gum inflammation and progresses from reversible gingivitis into periodontitis, where damage to the gum tissue, ligaments and bone becomes permanent.
Understanding which dogs are most vulnerable is the first step toward preventing irreversible damage.
I’m Sharon Milani, Co-Founder and Director of NutriFlex® and the formulator behind DentaMax™, a 100 percent pure organic Ascophyllum nodosum dental supplement developed specifically to address canine periodontitis risk factors through systemic plaque reduction. My work is grounded in evidence-based pet nutrition and ingredient transparency, aligned with South African regulatory standards.
With that context in place, let’s take a closer look at each of the key risk factors and what the research actually tells us.

Understanding Canine Periodontitis Risk Factors
To understand why some dogs lose their teeth by age five while others keep a pearly white smile into their teens, we have to look at the microscopic world inside their mouths. The primary driver of all dental trouble is the accumulation of bacteria. Within minutes of a professional cleaning or a good brush, a sticky layer called the salivary pellicle forms on the tooth surface. This pellicle acts like Velcro for bacteria, allowing them to latch on and create a complex community known as a plaque biofilm.
While visible tartar (calculus) looks unpleasant, the real danger lies in subgingival plaque. This is the invisible bacteria living below the gum line. When these bacteria thrive, they trigger an immune response from the dog’s body. Interestingly, much of the tissue destruction in periodontitis is caused by the dog’s own inflammatory response to the infection. You can find a deeper dive into this process in our guide on how dental disease develops in dogs.
Research into periodontal disease etiology and pathogenesis shows that once this biofilm matures, it becomes a “fortress” that is difficult to penetrate with chemicals alone. This is why dog dental disease explained usually focuses on the transition from gingivitis (inflammation of the gums) to periodontitis (destruction of the supporting structures). Gingivitis is reversible; periodontitis is not.
Genetic and Breed-Specific Canine Periodontitis Risk Factors
Genetics play a massive role in oral health. Some dogs are simply dealt a “bad hand” when it comes to their mouth anatomy. Brachycephalic breeds (those with shortened, flattened faces like Pugs or Bulldogs) often have the same number of teeth as a German Shepherd but packed into a much smaller jaw. This leads to severe overcrowding and rotated teeth, creating perfect “pockets” where food and bacteria hide.
Specific breeds are notorious for early-onset disease. Yorkshire Terriers are a prime example; research has shown that 98 percent of Yorkshires assessed already had mild periodontitis by just 37 weeks of age. Poodles also face high risks, with studies indicating that 100 percent of Poodles over the age of four are affected.
An interesting outlier is the Greyhound. Despite being a large breed, Greyhounds have some of the highest rates of periodontal disease. This is often attributed to a combination of genetics, a history of soft “racing diets” and a lack of early-life dental care in retired racers. For more on the unique challenges of smaller companions, see our articles on why small dogs have worse teeth and small dog teeth problems.
Environmental and Lifestyle Canine Periodontitis Risk Factors
While genetics set the stage, lifestyle factors often determine how fast the disease progresses. Dietary texture is a common point of discussion. While hard kibble provides some mechanical cleaning, it is rarely enough to prevent disease on its own, especially on the teeth used for shearing rather than grinding.
Home care compliance is perhaps the most significant modifiable risk factor. Daily brushing remains the gold standard, but in the real world, many owners struggle to maintain this routine. This lack of consistency allows plaque to mineralise into tartar within 48 to 72 hours. Furthermore, the frequency of professional cleanings matters. Waiting until a dog has “stinky breath” usually means the disease is already advanced.
Preventative strategies are essential for long-term health. You can explore how to prevent dental disease in dogs to learn more about balancing home care with professional intervention. Understanding the difference between plaque vs tartar in dogs is also vital for choosing the right tools for the job.
Breed and Size: Why Small Dogs Face Higher Risks
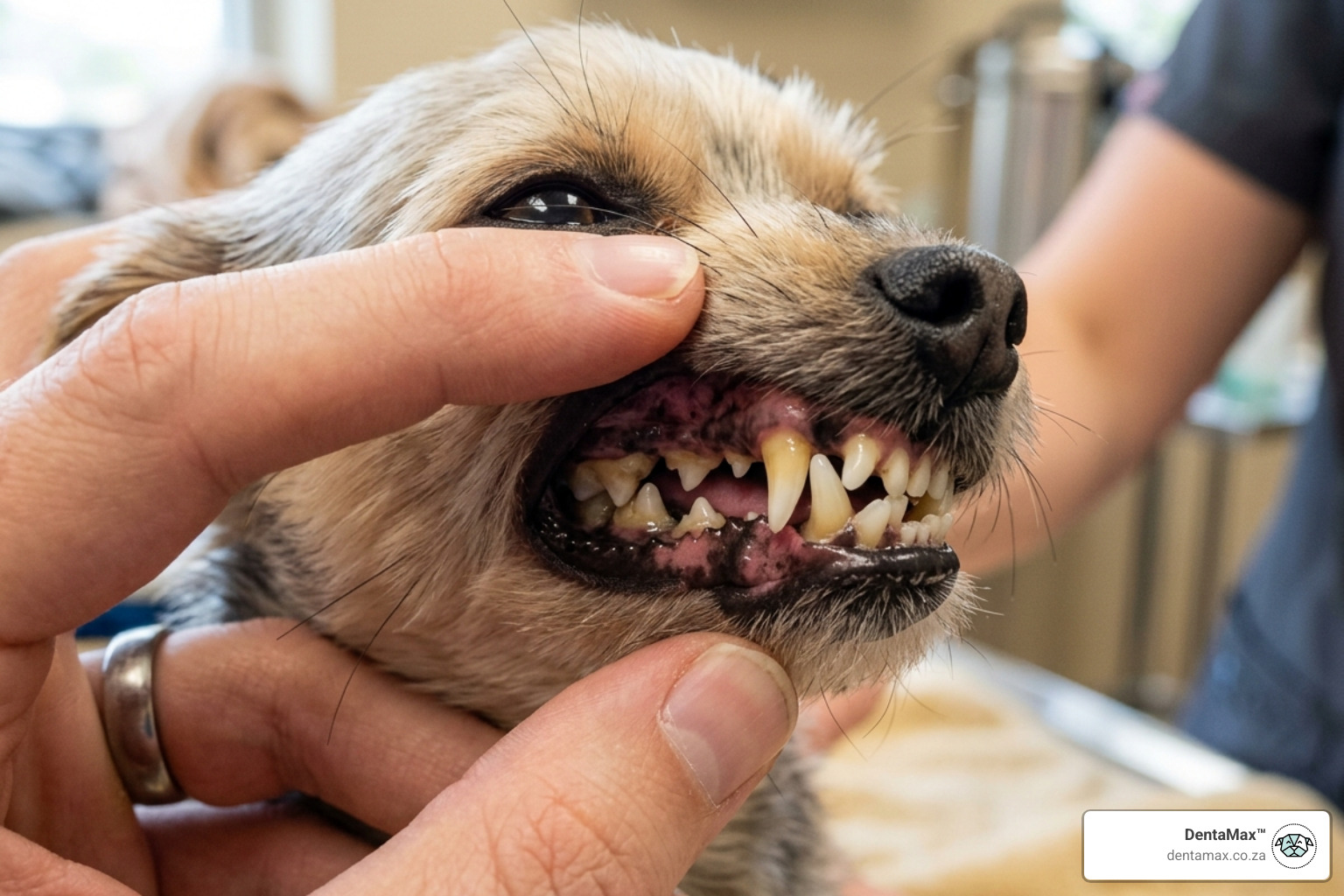
It is a well-documented fact in veterinary medicine: the smaller the dog, the bigger the dental bill. A massive study of over three million clinical records found that smaller breeds were 2 to 3 times more likely to be diagnosed with periodontal disease than larger breeds. In fact, 18 of the top 20 breeds with the highest prevalence were in the three smallest size categories.
There are several anatomical reasons for this:
- Tooth-to-Jaw Ratio: Small dogs have proportionally larger teeth relative to their jaw size. This leads to overcrowding, which prevents the natural “self-cleaning” action of saliva and tongue movement.
- Alveolar Bone Mass: Small dogs have much less bone surrounding the tooth roots. This means that even a small amount of bone loss due to inflammation can lead to tooth mobility much faster than in a large dog.
- Malocclusions: Misaligned bites are more common in toy breeds, leading to “traps” for plaque.
Scientific research on the frequency and impact of periodontal disease confirms that body weight is one of the strongest predictors of oral health. This is why we often emphasise why small dogs have worse teeth in our educational materials; these dogs require much more intensive preventative care from a young age.
The Role of Age and Body Condition in Oral Health
As dogs age, the cumulative effect of plaque exposure takes its toll. While gingivitis can be seen in puppies as young as 2 years old, true periodontitis usually takes hold between 4 and 6 years of age. By the time a dog is a senior, the damage is often extensive.
| Age Group | Estimated PD Prevalence | Clinical Focus |
|---|---|---|
| 1 to 3 Years | 80% (Gingivitis) | Prevention and training |
| 4 to 10 Years | 85%+ (Periodontitis) | Professional cleaning and X-rays |
| 10+ Years | 95%+ (Advanced PD) | Extractions and pain management |
Body condition is another critical factor. Recent research has shown that overweight dogs have significantly higher odds of a periodontal disease diagnosis. This may be due to the systemic low-grade inflammation associated with obesity, which can exacerbate the body’s inflammatory response in the gums. For owners of older pets, dental care for senior dogs should be a top priority during every veterinary visit. Further research on periodontal disease in dogs highlights that age and weight are uniform risk factors across almost all breeds.
Beyond the Mouth: Systemic Health Consequences
Periodontitis is not “just a mouth problem.” It is a source of chronic infection that can affect the entire body. When the gums are inflamed and bleeding, every time your dog chews, bacteria are pushed into the bloodstream (a condition called bacteremia).
The systemic risks are well-documented:
- Heart Disease: Bacteria from the mouth have been found in cardiac lesions and are associated with endocarditis and heart valve failure.
- Kidney and Liver Function: The constant filtering of bacteria and inflammatory markers can lead to chronic inflammation in these vital organs.
- Cytokine Release: The local inflammation in the mouth releases chemicals called cytokines into the blood, which can contribute to a state of systemic inflammation.
Symptoms like dog swollen gums or dog bleeding gums are early warning signs that the protective barrier of the mouth has been breached. If left untreated, this eventually leads to dog losing teeth, which is the body’s last-ditch effort to “shed” the source of infection.
Evidence-Based Strategies for Managing Periodontitis Risk
Managing canine periodontitis risk factors requires a multi-modal approach. You cannot rely on a single “magic bullet” treat; instead, you need a strategy that addresses both the mechanical and chemical aspects of plaque control.
- Mechanical Cleaning: Brushing remains the most effective way to disrupt the biofilm. Even brushing three times a week is significantly better than not brushing at all.
- Professional Intervention: An annual professional cleaning under general anaesthesia is necessary to reach the subgingival areas that a toothbrush cannot touch. This allows for scaling, polishing and essential dental X-rays.
- Systemic Plaque Reduction: This is where DentaMax™ and the science of Ascophyllum nodosum come in. Unlike mouthwashes that work on contact, certain compounds in this specific North Atlantic seaweed are absorbed into the bloodstream and excreted through the saliva. This alters the saliva’s composition, making it harder for plaque to stick to the teeth and softening existing tartar over time.
Research in the Revisiting Periodontal Disease Management review suggests that combining home care with nutritional support is the most effective way to delay disease progression. You can read more about how diet affects dog dental health to see how these systemic approaches fit into a South African pet owner’s routine.
Frequently Asked Questions about Dog Gum Disease
What are the primary clinical signs of periodontitis in dogs?
The most common sign is halitosis (bad breath), which is caused by the metabolic byproducts of bacteria. Other signs include red or bleeding gums, especially when chewing or playing with toys. As the disease advances, you may notice gingival recession (gums pulling away from the teeth), tooth mobility (loose teeth) and difficulty eating. Some dogs may paw at their mouths or drop food while eating because of the pain.
Why are Greyhounds considered a high-risk exception?
Greyhounds are an anomaly because they are large dogs with “small dog” dental problems. This is likely due to a genetic predisposition coupled with their racing history. Many retired racers were fed soft, raw “4-D” meat diets that provided zero mechanical cleaning. Additionally, dental hygiene is often not a priority in racing kennels, meaning by the time they are adopted at age 3 or 4, they already have advanced disease.
How often should my dog have a professional dental cleaning?
For high-risk breeds (small dogs and brachycephalic breeds), we recommend a professional evaluation starting at 1 year of age. For larger breeds, by age 2. Thereafter, an annual cleaning is standard. It is crucial that these procedures are done under general anaesthesia; “anaesthesia-free” dental cleanings are purely cosmetic and do not address the subgingival plaque that causes periodontitis. You can learn more about the progression of the disease in our guide to canine periodontal disease stages.
Conclusion
At DentaMax™, our mission is to empower South African pet owners with the knowledge to fight the “silent” epidemic of dental disease. By understanding canine periodontitis risk factors, you can tailor your dog’s care to their specific needs. Whether you have a tiny Yorkie in Johannesburg or a retired Greyhound in Cape Town, the goal remains the same: disrupting the biofilm before it disrupts their health.
Systemic dental science, particularly the use of Ascophyllum nodosum, offers a unique way to support your dog’s oral health from the inside out. By working through salivary excretion pathways, it provides a constant “anti-plaque” environment in the mouth, supplementing the work you do with the toothbrush. For more resources and evidence-based education, explore our dog dental disease explained category. Together, we can ensure our dogs live longer, happier lives with healthy smiles.

